CLICK TO EXPAND & READ TOPICS
Vaccinations
We vaccinate horses to help provide immunity against disease as part of an annual health plan. Timing of vaccination is dependant on various factors such as duration of immunity provided by the vaccine, expected exposure to specific viruses or bacteria and your horse’s current health status.
It is important to note the duration of protection provided by the vaccine as this will determine the timing of a booster vaccine. This can be especially helpful if you plan to be travelling or showing with your horse.
Vaccines work by stimulating the horse to “turn on” their own immune system. This allows for better ability to resist the agent when re-exposed in the future. We recommend vaccinating your horse 2-3 weeks prior to anticipated exposure.
The effectiveness of a vaccine can be reduced if your horse has poor nutrition, subclinical infection or is under severe stress. It is important to provide supportive care, such as good nutrition, proper housing, fresh water and a clean environment to help maximize your horse’s immunity and minimize disease exposure.
Influenza is one of the most common respiratory diseases in the horse, as it is highly contagious. The Influenza virus can be transmitted in the air from horse to horse by coughing or snorting, over long distances, as far as 30 meters.
The incubation period of Influenza in horses is typically 4-7 days. Clinical signs of infection in horses may include dry cough, nasal discharge, fever, depression and loss of appetite.
Rhinopneumonitis is transmitted by air and by direct contact with secretions, fomites or drinking water. The two most common virus strains, Equine Herpes Virus type 1 (EHV-1) and Equine Herpes Virus type 4 (EHV-4), are both known as Rhinopneumonitis. Both viruses may cause respiratory tract infections, fever, lethargy, loss of appetite, nasal discharge and a cough. In addition to these symptoms, EHV-1 may also cause abortion or neurologic disease.
Many horses contract this virus as foals from their dam, and some become asymptomatic carriers, intermittently shedding the virus at times of stress, throughout their lives. Young and elderly horses suffer most from respiratory tract infections, and may develop pneumonia secondary to the primary infection.
Although Tetanus is not contagious from horse to horse, it poses a constant threat to horses. Tetanus is caused by a toxin-producing bacteria which is present in the intestinal tract of many animals and found in abundance in the soil. The spores can exist for years and they enter the body through wounds, lacerations, or the umbilicus of newborn foals.
Symptoms include muscle stiffness and rigidity, flared nostrils, hypersensitivity, and the legs stiffly held in a sawhorse stance. As the disease progresses, muscles in the jaw and face stiffen which prevents the horse from eating or drinking. More than 80% of affected horses die.
The West Nile Virus (WNV) is transmitted when a mosquito feeds on an infected bird and then feeds on a horse. The virus is not directly contagious from horse to horse or horse to human.
The incubation period for WNV in horses is 3-15 days. Clinical signs of infection may include fever, incoordination, depression or anxiety, stupor, muscle weakness, partial paralysis, droopy lip, teeth grinding, muscle fasciculation, difficulty or inability to rise, convulsions, blindness or death.
The transmission of Eastern Equine Encephalomyelitis (EEE) and Western Equine Encephalomyelitis (WEE) is through mosquitoes to horses from wild birds or rodents, which serve as natural reservoirs of this virus.
Initial clinical signs include fever, stiffness and poor appetite, but after the incubation period of 1 -3 weeks, clinical signs develop into propulsive walking, depression, and sleepiness to aggression and excitability. The later signs can include head pressing, propulsive walking, blindness, circling, head tilt, facial and limb twitching, muscle tremors and recumbency, which is often followed by paralysis and death.
Strangles is a highly contagious bacterial infection, especially in younger horses due to their immature or naive immune systems. The bacteria, called Streptococcus equi subsp equi, can be spread by direct contact, by secretions from horse to horse or human to horse on hands, clothes, bedding, buckets, etc.
Strangles mainly affects the upper respiratory tract, but can spread to lymph nodes and other areas in the body. Clinical signs include high fever, depression, thick yellow nasal discharge, enlarged lymph nodes under the jaw and a productive cough.
Rabies is an uncommon viral infection affecting the neurological system of horses and other mammals. Although it occurs infrequently, the disease is fatal and poses serious human health risk. The virus is transmitted through the saliva (bite) of an infected (rabid) animal. Common host species include bats, raccoons, foxes and skunks. Common bite locations on horses are the muzzle, face and lower legs.
Clinical signs can be nonspecific but include colic, lameness, neurological symptoms such as ataxia, tremors and paralysis, fever, depression, increased sensitivity to touch and aggression. If you suspect your horse has been bitten by an animal listed above, do not make direct contact and contact your veterinarian immediately.
Dentistry
An oral examination should be an essential part of an annual physical examination by a veterinarian. Every dental exam provides the opportunity to perform routine preventative dental maintenance. The end result is a healthier and more comfortable horse. Through examination, more serious dental problems may be identified, such as ulcers of the cheeks or tongue, infections of the teeth and gums, extremely long hooks or overgrowths on the cheek teeth, and lost or fractured teeth.
Routine maintenance of a horse’s teeth has been historically referred to as “floating.” Because the horse’s lower rows of cheek teeth are closer together than the upper rows of cheek teeth, and the horse chews in a sideways asymmetrical figure eight motion, sharp points form along the edges of the cheek teeth. These points should be floated to prevent damage and ulceration of the cheeks and tongue as well as other periodontal diseases.
Clients often ask, “What happens to horses in the WILD?” The most common differences are:
- Horses have been selectively bred for thousands of years for various criteria including size, colour, strength, athleticism, but not for good dental conformation
- Horses ‘in the wild’ subsisted on poor quality range pastures, high in roughage, not soft hays, pellets and grains we feed them today
- Domesticated horses’ life expectancy is much longer, probably double that of their wild counterparts. Today, many horses are outliving their teeth!
- Horses have an expected level of performance under saddle, and we ask them to have soft and supple contact in the bit.

(a) Equine Odontoclastic Tooth Resorption and Hypercementosis (EOTRH) is a very painful dental disease that has just recently been diagnosed by veterinarians. This disease primarily occurs in horses 15 years or older. The bone and tissue around the incisors, and sometimes the canines, become inflamed and start to dissolve. Some roots deposit excessive cementum creating a calcified bulb appearance. As the disease progresses, infection develops and causes the teeth to loosen. Owners may notice swellings or pimple like red dots on the gums near the teeth roots. Horses may not want to bite down on hard treats such as apples or carrots, or start to lose interest in grazing. The sooner this disease is caught, the better the outcome.
(b) A missing or damaged tooth can, over time, cause dental issues. As the normal teeth continue to erupt, they have opposing teeth to evenly wear each other down. The problem occurs when the opposing tooth of the missing or damaged tooth continues to erupt and does not get worn down as the others do. This overgrowth will cause pain and injury to the soft tissue in the mouth, prevent the horse from chewing normally, and predispose it to developing many other dental abnormalities.
(c) Supernumerary or ‘extra’ teeth are rare, but can cause problems especially if they are unopposed. It is crucial that the overgrowths are reduced at least two to three times a year or are extracted to prevent pain and injury to the soft tissue in the mouth.
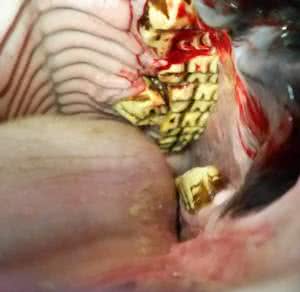

Common Signs of Equine Dental Discomfort or Disease:
• Quidding (dropping feed)
• Reluctance to bite hard treats, apples or carrots
• Inflamed gum line or small red dots above the gum line
• Foul smell coming from the horse’s mouth
• The appearance of swollen cheeks
• Loss of appetite
• Behavioural issues when in a bridle
• Head shaking
• Weight loss
• Choosing to eat fine and soft hay over course hay
• Nasal discharge coming out of one nostril

Equine Odontoclastic Tooth Resorption and Hypercemetosis, or EOTRH for short, is a progressive and painful dental disease of the incisors and occasionally canine teeth in horses. The roots of affected teeth begin to reabsorb and can develop bulbous deposits of cementum (one of the components of teeth) around the roots which then cause the bone around the tooth to painfully deform. EOTRH is still not completely understood, and we don’t entirely know what triggers the start and progression of this disease. What we do know about EOTRH is it occurs in middle-aged to older horses and is far more common in male horses than females.
Signs your horse may have EOTRH:
- Weight loss
- Discomfort wearing a speculum during routine dental float
- Hesitation to bite hard treats (like carrots or apples) with the incisors
- Head shy or specifically mouth-shy behaviour
- Lost or loose teeth
- Draining tracts around the incisors
- A “Lumpy” appearance to the gingiva around the incisors
- Reactivity to being bridled or taking consistent bit contact
An oral exam of affected horses often reveals gingival recession, gingivitis (often with red dots on the gingiva around affected teeth), draining tracts from abscessed teeth, and a bulbous or lumpy appearance to the bone and tooth roots. EOTRH is diagnosed by taking radiographs of the incisors and canine teeth and looking for signs of resorptive lesions, bulbous growths around the roots, and bone loss around the tooth roots. The only treatment for these painful teeth is to extract them and eliminate the on-going source of pain. Often the horses affected by EOTRH are very stoic and hide the fact that they are living with significant dental pain. Because of this, many owners struggle with the thought of removing all the affected teeth. However, once those painful teeth are removed these horses often “come back to life”: gaining back lost weight, becoming less head shy, eating voraciously, and grazing on all but the shortest grass. The recovery from extractions is typically straight forward and only requires rinsing feed from the extraction sites regularly while they fill in with granulation tissue. In these post-extraction patients after their recovery, often the only way you can tell they’re missing any teeth is by the tip of their tongue that hangs out from between their lips!

Parasites
- Three major species include Strongylus vulgaris (up to 25 mm), S edentatus (up to 40 mm), and S equinus (up to 50 mm)
- The larvae develop to the infective stage within 1–2 wks after the eggs are passed
- Ingested infective larvae hatch in the intestine and migrate extensively through the body before developing to maturity in the large intestine. This process takes 6–11 months
- The larvae travel through the liver, blood vessels, pancreas and other parts of the abdomen causing damage along their routes
- Small Strongyles’ early development is confined to the wall of the intestine
- They feed on the mucosal lining of the intestines sometimes causing severe ulcers in the wall of the colon
- In heavier infections, damage may be extensive enough to disturb digestive and absorptive function, resulting in loss of condition and diarrhea
- In one of their larval stages, they encyst in the mucosal lining of the intestine, evading the drugs targeted at killing them
- The botfly does not actually bite or cause direct pain to the horse
- The botfly lays its eggs, which are small, round, and yellow-orange in colour, on the horse’s skin of the inner legs and knees, around the chin and nose, and on the belly then waits for the horse to ingest them.
- They remain in the horse’s mouth for about four weeks before migrating to the stomach.
- The larvae stay in the stomach, where they attach to the gastric lining for approximately 8-10 months until maturity, and then pass in the horse’s feces.
- Tapeworm eggs are passed in the manure where forage mites ingest them
- Horses ingest the mites infected with the tapeworm larvae, releasing the tapeworm
- Within 6-10 weeks, the immature tapeworm develops into an adult, attaches to the horse’s intestine and causes damage to the intestinal mucosa and nerve degeneration at the site of attachment
- Large numbers of attached tapeworms can obstruct the bowel; however, even light to moderate infections have been associated with impaction, spasmodic colic, obstruction and rupture
- The ascarid, or roundworm female can lay 100,000 to 200,000 eggs in one day
- Infective larvae develop within the eggs and remain viable for up to 10 years in the environment
- They are common in all foals and weanlings and can cause serious impaction colic, poor thrift, respiratory disease, rough hair coat and diarrhea
- Foals require a frequent deworming protocol until they are at least 9 months old
- Pinworm adults crawl out of the horse’s rectum to lay their eggs, which can cause intense itching and hair loss around the tail head
- Pinworm eggs hatch on the horse’s skin, then crawl back into the rectum
- Because pinworms spend their entire lives in the large colon and rectum, they cause very little damage to the horse other than irritation and self inflicted trauma
- In addition to deworming, the perineum, tail and surrounding areas should be thoroughly washed to remove all eggs recently deposited by the pinworms
- Anthelmintic resistance is the ability of worms in a population to survive treatments that are generally effective against the same species and stage of infection
- Adult horses vary greatly in their innate susceptibility to infection and their level of egg shedding and thus, require individualized attention to their parasite control needs
- Horses less than about 3 years of age also require special attention as they are more susceptible to parasite infection, and are more at risk for developing disease
- Fecal egg counts are used to select only those horses with moderate and high egg shedding for anthelmintic treatment
- Only 20-30% of horses tend to be moderate or high egg shedders
- In traditional deworming programs, repeated treatment of low shedder horses every 2-3 months accomplishes little to improve their health, but it does promote drug resistance
- Identifying and selectively treating only moderate and high shedding horses helps protect the entire herd from developing and contracting drug resistant parasites
A fecal egg count is a microscopic examination of fresh manure for parasite eggs, which allows the veterinarian to determine which parasites are present and the load of the infection. This information is very important in developing an appropriate deworming program for your horse or herd, and in monitoring the effectiveness of the program. However, it is important to note that a negative fecal egg count does not mean your horse is free of internal parasites because some parasites only produce eggs intermittently or not at all. Therefore consultation with your veterinarian to determine who to test, when to test, when to treat and with which dewormer is essential for herd health and the fight against anthelmintic resistance.
Collecting a fecal sample for testing involves collecting 2-3 fresh manure balls in a labelled ziplock bag. The collected manure balls needs to be fresh, as in warm, and should be from the centre of the pile where it has not been contaminated by the ground or flies on top. Once the sample has been collected, it should be taken to the SEVS office for testing immediately. If not, the sample needs to be refrigerated overnight until it can be dropped off.
(a) Differentiating between dewormer brands and drugs can be very confusing since there are many brands available to horse owners. Owners need to be careful that they are alternating between different drugs, and not simply alternating between different name brands of the same drug. Please see below a list of brand names versus drug:
1. Drug: Fenbendazole; Brand names: Panacur, Safeguard
2. Drug: Moxidectin; Brand name: Quest
3. Drug: Pyrantel Pamoate; Brand names: Stongid P, Strongid T, Exodus
4. Drug: Ivermectin; Brand names: Eqvalan, Bimectin, Panomec
5. Drugs: Moxidectin & Praziquantel; Brand name: Quest Plus
6. Drugs: Ivermectin & Praziquantel; Brand names: Eqvalan Gold, Equimax
(b) Individualized programs are very important to develop through consultation with your veterinarian. Veterinarians can help determine who requires treatment, when to treat, with which dewormer, and at what time of year.
The American Association of Equine Practitioners has published general guidelines for parasite control. These guidelines provide a comprehensive set of recommendations for helping veterinarians develop improved strategies for parasite control in horses of all ages.
Equine Diseases
Pituitary Pars Intermedia Dysfunction, aka Equine Cushings Disease, is most often seen in older horses (>14yrs), but can occur in younger horses as well. The disease is caused by changes in brain chemistry which affect the pituitary gland, increasing the amount of a hormone, called ACTH, being produced and released into the horse’s body.
Symptoms of PPID include:
- Laminitis/founder
- Fat deposits at the tail head, behind the shoulder, the crest of the neck
- Loss of topline muscling
- Long hair coat, or delayed shedding of the winter coat
- Abnormalities with sweating
- Lethargy or change in attitude
- Increased water intake and urination
- Recurrent or persistent infections
Testing for PPID is easily done with a blood test for circulating levels of ACTH. This test is most sensitive in the fall.
While any breed may develop PPID, pony breeds and Morgans are predisposed.
Although PPID is not a curable disease, treatment with a daily dose of an oral medication can control the symptoms. Promoting weight loss and decreasing the sugars in your horse’s diet by choosing hays low in sugars (non-structural carbohydrates), switching to a low-starch grain or eliminating grain from the diet entirely, and limiting access to pasture will decrease the risk of laminitis and help your horse thrive despite this disease.
Insulin Resistance, or Equine Metabolic Syndrome, is a condition of unknown cause that affects middle-aged, overweight horses. Similar to humans with type II diabetes, these horses do not respond normally to the insulin produced by their body.
Symptoms of Insulin Resistance include:
- Laminitis
- Obesity
Testing for Insulin Resistance is easily done with a simple blood test.
While there is no direct treatment for insulin resistance, horses with this condition need a low-sugar diet and regular exercise. Hays low in sugars (non-structural carbohydrates) and a low-starch grain while removing all access to grass are key to decreasing the risk of laminitis in insulin resistant horses.
Medications to increase your horse’s metabolism are helpful in cases of overweight horses with insulin resistance.
Regular exercise to burn any stored or circulating glucose, and encourage weight loss is equally important. Fat cells store many inflammatory mediators that encourage propagation of inflammation throughout the body, which leads to the desensitization of tissue to insulin as well as the inflammation of the laminae in the feet. So by eliminating excess fat cells we can actually prevent the progression of the disease.
For more detail about how to feed a horse with IR, please see our Care Instructions section.
Horses can suffer from allergic airway diseases, commonly termed Equine Asthma. Intermittent Airway Disease (IAD), describes a condition most often seen in young horses who exhibit some exercise intolerance and/or cough during exercise but are normal at rest. They can recover spontaneously or with treatment. Recurrent Airway Disease (RAO), used to be termed COPD or heaves, describes a more chronic condition with narrowing airways (bronchoconstriction), bronchospasm, and mucous production. These horses are not normal at rest. They exhibit a chronic cough, exercise intolerance, increased respiratory rate, nasal discharge, and respiratory difficulty. Horses afflicted with this condition will develop a “heave line”, a distinct line along the flank created by increased abdominal muscles which help the horse breathe.
RAO occurs from the lung’s hyperreactivity to inhaled allergens, and similar to human asthma, it has underlying allergic and inflammatory components. The average age on onset is between 9-12 yrs old and approx. 12% of mature horses are affected. There is no breed or gender predisposition, but it does seem to have a heritable component.
For most horses, the disease is seasonal as symptoms are exacerbated by certain triggers seen at certain times of year. Horses affected primarily in winters months are often hypersensitive to moulds, decomposing organic matter, hays and straw allergens. Horses affected primarily in summer months are most sensitive to pollens and dust
Diagnosis of RAO is based on medical history, respiratory exam findings, and inflammatory cells found within the trachea or bronchi, without the presence of infectious agents. The most important treatment strategy is the identification and elimination of the allergen triggers through environmental and dietary changes to reduce or remove moulds and dusts. If these management changes do no alleviate symptoms, or if the lung disease is advanced, medications to control the inflammation and bronchoconstriction are employed.
Unfortunately, RAO is a chronic disease that will need to be strictly managed throughout the horse’s life. Some key management strategies for horses with IAD or RAO include:
- Soaking hay and feed in water will reduce dusts and some moulds. * May exacerbate symptoms in severely affected horses
- Steaming hay will add moisture to the hay but also by raising the temperature, will better eliminate mould spores.
- Avoid round bales. Round bales have much higher concentrations of dusts and moulds, and horses submerging their heads into round bales will breathe them in.
- Switch to pelleted or cubed feeds.
- Feed horses from the floor to increase mucous drainage.
- Turnout on dust-free pasture as much as possible.
- If horses must be stalled, make sure it is well ventilated, even in winter.
- Avoid storing hay in lofts above stalls.
- Do not bed on straw or shavings (the entire barn).
- Clear out the barn before cleaning. Wet down aisles and avoid leaf blowers to reduce aerosolization of dusts and moulds. Wait at least a few hours before bringing them back in.
- Thoroughly clean out the rafters and under the stall mats at least twice yearly to remove decomposing organic matter.
- Exercise horses on moist, dust-free footing.
EC Rules and Regulations
Equestrian Canada (EC) encourages equestrians in all sports to participate in anti-doping measures and fair medication control to safeguard the health and welfare of horses. However, we often receive conflicting information regarding what can and cannot be given to our equine athletes during an EC sanctioned horse show. Please click here for the latest guide from EC.
This handy guidebook gives the approximate length of time that some drugs can be detected in the blood and urine of horses. It can be helpful to determine the elimination of certain drugs and medications when you are scheduled to compete in an EC sanctioned show. Please click here to access this guide.
Equine Conditions
Various aspects of the horse’s anatomy and physiology, combined with common husbandry practices, make the horse prone to developing gastric ulcers. Horses continuously produce acidic digestive juices within their stomach, at a rate of 1.5L per hour in the average horse, whether they are eating or not. Horses evolved to graze nearly continuously, and as such their stomachs are designed to always be receiving feed. When a horse is grazing, or eating hay continuously at a slow rate (like from a slow-feeder hay net) there is a regular supply of feed and saliva into the stomach. A horse that only has access to feed for a short period every day still produces the same amount of acid as the grazing horse, but has far less buffering capacity in feed and saliva, and therefore a more acidic environment within their stomach.
Known as Equine Gastric Ulcer Syndrome (EGUS), there are two main varieties of gastric ulceration in the horse. The distinction is made based on the location of the ulceration within the stomach and the triggering causes of the two varieties of EGUS are thought to be different. The equine stomach is divided into two sections, based on the type of tissue which lines the stomach walls. The upper portion of the stomach where the esophagus enters, is covered with squamous epithelium, and for simplicity’s sake can be considered an extension of the esophagus with no protection against acidic gastric fluid. The lower portion of the stomach is lined with glandular epithelium, which secretes the acidic digestive juices. This glandular epithelium provides itself protection against the highly acidic environment through mucous and buffers held close to the surface of the tissue. Ulceration of the upper portion of the stomach is called Equine Squamous Gastric Ulcer Syndrome (ESGUS), while ulceration of the lower portion is known as Equine Glandular Gastric Ulcer Syndrome (EGGUS). The most common location for ESGUS is along the dividing line between the squamous and glandular epithelium, which is known as the margo plicatus.
The prevalence of EGUS ranges from 50-90%, depending on the population considered. The symptoms of EGUS are highly variable, which makes it difficult to identify horses affected by this syndrome without further diagnostics. Horses with EGUS may display one or more of the following symptoms:
- Recurrent colic
- Decreased appetite (particularly for grain)
- Diarrhea
- Poor weight gain, or weight loss
- Low-grade anemia
- Teeth grinding
- Cribbing
- Low energy
- Poor hair coat
- “Girthy” behaviour
- Bucking
- Irritation to leg aids
- Unwillingness to go forward, particularly at faster gaits
- Refusing jumps or specific movements
The best way to determine if your horse has EGUS is to perform gastroscopy. This procedure involves passing a long camera through the nose, into the esophagus and then the stomach. This allows for a visual evaluation of the stomach lining for signs of ulceration. This procedure can be done on-farm with sedation similar to that required to float their teeth, and requires an hour or less to complete.
If your horse is diagnosed with EGUS, treatment for the condition involves decreasing the acidity in the stomach through several means. The most effective means is via acid-suppressing medications like omeprazole (Gastrogard). Omeprazole is absorbed in the small intestine and works on the acid-secreting cells of the glandular stomach via the blood stream to decrease the amount of acid produced. The resulting decrease in acidity provides the lining of the stomach a gentler environment, better suited for healing. Other medications can be combined with omeprazole therapy depending on the individual situation.
Medication for EGUS is typically used in combination with modifications to the horse’s diet and lifestyle. Increasing the amount of forage in the diet, and chewing time with slow-feeder hay nets, helps provide a buffer against the acidic gastric fluid by the bulk of hay within the stomach as well as increased production of saliva, which buffers the stomach acid. High grain meals increase the acid production in the stomach and should be avoided or minimized as much as possible. Stress and high intensity exercise are associated with increased risk of EGUS, and efforts should be made to reduce or accommodate for both of these in your horse’s lifestyle. These changes in lifestyle are useful preventative measures as well, and should be continued even after the treatment course is finished.
If you are concerned your horse may be affected by EGUS, please call our office to discuss your horse’s situation and schedule a consult.
One of the most infuriating conditions in the horse is skin problems. Frustrated owners can be brought to tears watching their unlucky horse suffer with Sweet Itch, a common skin condition that, so far, has no cure.
Sweet Itch, also known as Insect-bite Hypersensitivity, is an allergic reaction to the saliva of biting midges called Culicoides, better known as “No-See-Ums”. The allergic reaction can cause intense itching and bumps along the mane and tail head as well as the belly of horses. Many horses are so overwhelmed by the intensity that they throw themselves on any surface available, rubbing their manes and tails on trees, fence posts and boards. Some horses will ‘dog sit’ rubbing their bellies in the dirt and gravel. These behaviours can lead to abraded skin wounds, imbedded foreign material and secondary infections, intensifying the irritation and propagating the self-trauma. Horses suffering from relentless itching, and painful skin infections are also prone to other physiological conditions such as sleep deprivation, fatigue, irritability and even gastric ulcers.
Management of this problem a very frustrating for owners as well. In order to control it, treatment needs to start BEFORE the horse starts exhibiting signs, so that the allergic reaction and level of itchiness has not had the chance to flare. Once the immune system has been triggered into over-reaction and hypersensitivity, controlling the itchiness and preventing the horse from scratching and propagating the reaction it extremely difficult.
Here are some of the management strategies:
1) Limit standing water which attracts midges and provides their breeding ground and refresh water buckets frequently
2) Bring your horse inside when midges are most active at dawn and dusk
3) Install fans in the stalls and barns
4) Invest in a Sweet-Itch blanket that covers nearly the entire body
5) Place fine mesh screens over barn windows, doors and other openings
6) Apply insect repellent very frequently
7) Feed Omega fatty acids found in flax oil, hemp oil and camelina oil
8) Feed Vitamin E and Zinc for skin support
9) Apply thick topical creams such as Vaseline, zinc cream, “Bag Balm” to act as a physical barrier
10) Apply soothing creams and ointments on irritated skin
11) Administer antihistamines to suppress the body’s allergic reaction
12) Employ desensitization immunotherapy during the non-reactive months to reduce your horse’s sensitivity to midge saliva
There is no cure for this condition, so prevention and early treatment are key to keeping your horse comfortable during the spring and summer months. The midge season is typically April thru September, and the midges are most active at dawn and dusk. So start treatment early April before the midge has a chance to bite your horse.
Equine Care
Colic, or abdominal pain, is a common emergency we often see with the changing of the season. Although some horses’ clinical signs of colic are painfully obvious, triggering the owner to call the veterinarian right away, others exhibit mild signs, reflecting a mild colic, which can resolve with a little change in management and care, and without a visit from the vet. The challenge is that some horses’ mild colic signs DO NOT reflect the severity of the colic, which can result in death of the horse if treatment is delayed.
Signs of colic can include any number of the following: a reduced or lost appetite, reduced or absent manure production, change in gut sounds (reduced, absent or increased), change in mucous membrane colour or moisture, looking at sides, stretching, pawing, sweating, trembling, lying down, or rolling. Some horses exhibit unusual signs in response to pain such as exhibiting the flehmen response, gorging on food or running away from the pain. Some horses’ signs are so mild, they are hardly evident.
Colic does not discriminate in age, sex, breed, discipline, or environment. Any horse can colic, and most have at least one episode of colic in their lives. Although 90% of colics can resolve with medical or surgical care, owners must be attentive, identify signs of colic quickly and act appropriately.
Here are 10 DOs and DON’Ts when it comes to colic:
- DO take your horse’s vital signs: Rectal Temperature, Heart Rate, Respiratory Rate and Gut Sounds.
- DO look for the presence, volume, number and consistency of manure in your horse’s stall and paddock.
- DO call the vet immediately regardless of the severity of signs. Have the vital signs and manure information ready to share with the vet.
- DON’T ‘Wait and See’- Delaying treatment can turn mild colic into severe colic and severe colic into untreatable colic.
- DO closely monitor your horse. Do not go and run errands for a few hours and then check back. Colic can turn from mild to severe within 15 to 20 minutes, so make sure to check on your horse every 15 to 20 minutes.
- DO walk your horse if it is safe to do so and advised by the vet to stimulate gut motility and prevent rolling.
- DON’T exercise your horse vigorously as it can exhaust and dehydrate the horse.
- DON’T offer feed or water unless advised by the vet
- DON’T medicate without permission from your vet. Medicating before the exam can mask signs and delay proper diagnosis and treatment.
- DO start thinking about trailering options if referral to a hospital or surgical facility is warranted. Time delays to organize transport can affect the outcome.
The “Take Home Message” is to call the veterinarian at the first signs of colic so that we can determine if your horse can be monitored and managed by you initially or if it warrants a visit right away. DON’T make the mistake of assuming mild signs = mild cause of colic. DO call us immediately at (250) 588-9438 and DON’T text or email.
As travel season quickly approaches it is time to prepare your trailer, yourself and your horse for trailering. First off, it’s time to scrub the moss off that trailer and give it a once over or even take it into a mechanic to do annual maintenance before loading your horse up. Then start planning your travel or show schedule keeping in mind the distance, weather and road conditions and your horse’s stress level with trailering.
Horses often do well on short day trips when they have been well acclimatized to trailering, but we can make it an even more positive experience by planning the best route without delays, tricky corners or bumpy roads. Inside the trailer we can also make the experience more pleasant and healthy by adjusting the windows, fans and doors to create a comfortable temperature. If you’re trailering with another horse keep the horses within sight of each other while loading. When you unload allow your horse time to graze and take in the new scenery. This can become a routine that the horse will become comfortable and happy with.
Longer hauls require much more planning and caution. Prior to the trip become familiar with your horses baseline temperature, heart rate and respiratory rate so that they can be monitored throughout the journey.
Horses do best when their routine is maintained so the goal is to keep your horse’s day as close to normal as possible. This is difficult when you have your horse in a trailer for the majority of the day, but bringing enough of your own hay, grain and supplements will help. Also try to keep feeds at the same time of day as usual.
Dress your horse for the journey. Using a head bumper protects the horse’s head in cases of sudden stops or if the horse tosses his head. Proper shipping bandages that cover the coronary band are also important to protect your horse from injury. Ideally, have your horse in a leather halter or use a quick release clip in case your horse falls backwards. When you tie your horse he should have enough room to use his head and neck for balance and stand in a comfortable position for an extended period of time. He should be able to touch the rear bar or wall so he can be aware of his parameters.
Tie a hay bag rather than a hay net to prevent dust and mold spores from blowing directly into your horse’s airway. If you use a hay net try soaking the dust and mold spores out of the hay prior to hanging it and hang it as low to the ground as possible without creating risk of a caught hoof. This will minimize the risk of contracting a respiratory infection commonly called, “shipping fever”. Trailer bedding should be cleaned regularly to prevent respiratory issues shipping. Bedding pellets are often recommended because they absorb a lot of liquid and are dust free.
Provide water to your horse every 3-4 hours. If your horse is finicky about drinking water away from home you can either bring the water supply for the trip or a few days prior to leaving start experimenting with adding different flavours to the water, such as Kool-Aid, molasses, peppermint flavouring or apple juice. Once you find your horse’s preference add it to the water at the new location. You should however, always bring at least 20 gallons of water on both long and short trips so it can be used for drinking, treating possible wounds, or cooling your horse off.
When you make it to rest stops offer a drink of water and assess the air quality in the trailer and adjust the windows, doors and fans accordingly. Try to avoid prolonged stationary periods in traffic, at refueling stops or border crossings. A trailer in the sun can be more than 20 degrees warmer inside than outside.
Having a portable first aid kit is a necessity while travelling with your horse. Here is a list of items that you will need to build your own.
A five gallon bucket with a lid (Dual purpose: container to hold all the items and it can be emptied to use for first aid purposes like washing wounds)
Telfa Non-Stick Pads
Vetwrap
Syringes
Gauze
Epsom Salts
Thermometer
Stethoscope
Scissors
Tweezers
Duct Tape
Animalintex
Gloves
Small Towels
Hand Sanitizer
Flash Light
Alcohol Preps or small container with gauze and rubbing alcohol
Betadine
Chlorhexidine Scrub
Antibiotic Ointment
Water
Antiseptic Wound Spray
Also, talk to your vet about adding prescription medications to the kit like anti-inflammatories, analgesics, and tranquilizers.
Choke is not an uncommon problem in horses, particularly in those with poor teeth or those who eat faster than they chew. While in horses a choke is still a medical emergency, it is not as scary as what many of us initially envision. In horses, choke describes a blockage in the esophagus, not in the trachea. Because of this, a horse who is choked can still breathe. However, a choke should still be dealt with promptly, as the condition is painful and stressful for your horse, and a choked horse has a high risk of aspirating feed and saliva into the trachea, putting them at risk of developing pneumonia.
The classic signs of a choke are coughing, retching, an extended neck posture, saliva +/- feed material draining from the nostrils, an unwillingness to eat, and stress or anxiety. Often your horse will show some or all of these behaviours in the middle of a meal, or shortly thereafter. If you suspect your horse may be choking, remove their feed and water, keep them calm and their head as low as possible to allow saliva and feed to drain out of their nostrils, and call your veterinarian. In some cases mild chokes will resolve on their own, but often the horse requires medical attention to dislodge the blockage in their esophagus.
Your veterinarian will sedate and pass a nasogastric tube through the horse’s nostril into their esophagus. Through a combination of gentle pressure and repeated rinsing of water, your vet will remove the blockage. Thankfully serious complications such as pneumonia are rare when chokes are treated in a timely manner.
Are You a New Horse Owner?
Congratulations on your new horse ownership! Having a new horse is always exciting but requires careful planning to provide your horse with consistent and diligent care. As a new horse owner you will find that you never stop learning. The following are key areas of information to get your knowledge base started.
VETERINARY CARE
Routine veterinary care usually requires 1 – 2 farm calls per year; the first for the annual physical exam, vaccinations and potential dental care (if the horse requires it at that time), the second is for booster and/or seasonal vaccinations and potential dental care (if the horse did not require it at the previous visit). Topics on general care and medical concerns can be discussed at the exam, as well as addressing any questions or concerns you may have.
DENTAL CARE
Regular dental care will help your horse maximize nutrient availability in their feed and prolong the use of his teeth into old age. It is recommended to have your horse’s teeth checked once a year at an annual exam. If the enamel points are sharp or if there are any other issues, they can be corrected at that time. Maintaining regular dental care can improve your horse’s behaviour, bit comfort, trainability and performance. Having regular dental checks promotes early diagnosis and treatment of dental disease.
VACCINATIONS
The American Association of Equine Practitioners (AAEP) recommends a core group of vaccines to be administered by your veterinarian annually. However, a standard vaccination program for all horses does not exist. The following criteria is used to determine your horse’s vaccine needs and schedule:
- Risk of disease (geographic factors, age, use)
- Consequence of disease
- Anticipated effectiveness of the selected vaccine
- Potential for adverse reaction to vaccine
- Cost of immunization vs. potential cost of disease (treatment, loss of life)
DEWORMING
Up to date research recommends individualized parasite treatments for your horse based on parasite type and load, rather than indiscriminate deworming treatment. Assessing your horse’s parasite infection can be done with a simple fecal egg count (FEC). Contact our office for fecal collection instructions. The FEC results assist the veterinarian in determining whether it is appropriate to deworm your horse, and with which medication.
COMFORT
Is your horse comfortable? Causes for discomfort can range from musculoskeletal disease to tack and equipment ill fit. Depending on the age of your horse and his job, you may want to speak to the veterinarian about various options for joint health maintenance, to help support your horse’s performance and longevity. Determining whether your saddle and bridle is well-fitted to your horse is often a team effort – enlisting a coach or trainer can often be a good first step, but it may require additional guidance from a saddle fitter or veterinarian.
HOOF CARE
Horses’ hooves grow continually and require frequent trims/shoeing to maintain balance and health, to avoid pain, unnecessary force on joints and ligaments, as well as unequal compression on hoof structures, bone and cartilage. Hooves grow more slowly in the winter and may only need trimming every 6-8 weeks, compared to the summer when they may require trimming every 5-8 weeks. Your horse’s trim or shoe cycle length should be recommended by your farrier and/or veterinarian. Veterinarians and farriers often collaborate to best assess your horse’s hoof care needs.
COST
The dreaded and uncertain reality of equine costs is extremely important to consider for your horse’s health and your financial planning.
For basic veterinary care: annual physical exam, dental care and vaccinations is approximately $400 to $600 per year per horse. This does not include the cost of emergency services, such as life saving treatments for colic, which can range from $500 to over $10,000 (if surgery is required). Nor does it include treatment for chronic conditions, such as osteoarthritis, allergies or PPID, which can range from $300 to $1500 annually.
Regular farrier services will range depending on your horse’s trim/shoe cycle and your farrier’s costs, but it will likely range from about $400 to $2300 annually. This does not include the extra farrier visits for a pulled shoe or a hoof abscess.
The cost for board in Victoria ranges depending on how many services the boarding facility offers. Barns with self-board or co-op board provide the facility and the owner or owners are responsible for sourcing feed, feeding and general husbandry. Cost for this kind of facility ranges from about $250 to $550 per month, and does not include the cost of feed, bedding, etc. Full board includes the facility, feed and husbandry which ranges in cost from about $550 to $1000 per month. There still may be added fees for anything outside of general husbandry such as specialized feeds, blanket changes, or medication administration.
Lameness and Hoof Pain
As the winter wet starts up, our horses – particularly their feet – are exposed to wet, mucky conditions once again. A risk of these conditions is the development of a hoof condition called thrush. Thrush is often a mixed infection of bacteria and/or fungus in the frog tissues of horses’ hooves. Horses that live in stalls or small paddocks are more likely to develop thrush, as are those with deep, narrow sulci (grooves) alongside and in the center of their frogs. Deep, narrow sulci allow moisture and bacteria-containing debris to accumulate next to the frog tissue, exposing it to infection. Often thrush infections are superficial and do not cause the horse pain. The tell-tale sign of thrush is a dark, pasty discharge from the sulci of the frog, often with an offensive odour. Some cases of thrush can progress to the point of infection of the deeper, more sensitive tissues of the frog causing lameness and the tissue may bleed easily when the hooves are picked.
Treating thrush starts with ensuring moisture and debris are not regularly trapped alongside your horse’s frog. This involves regularly picking their feet, having your vet or farrier trim the horse’s frog to minimize how deep and narrow the sulci are, and ensuring the horse has a clean, dry area to stand. Many cases also require treatment with topical antibacterial/antifungal products. Dilute iodine, dilute bleach, or commercial products such as Thrush Buster all serve a similar purpose to kill the organisms responsible for the infection. More severe cases may require more in-depth treatment, contact your veterinarian if you are struggling to make headway with your horse’s thrush.
The best treatment for thrush is prevention. Do your best to ensure your horse’s turnout has good drainage and is mucked out regularly to limit mud and wet manure accumulation. Ensure they have clean, dry areas to eat and rest in. Picking your horse’s feet out daily is a great way to help prevent thrush and to regularly evaluate the hoof for any early signs of the condition allowing for early treatment.
Osteoarthritis (OA) is an all-too common ailment of athletic horses everywhere. Many times thought of as an “old horse disease”, OA can affect horses of any age, and research indicates about 60% of all lameness is related to OA in athletic horses. OA is a multifactorial disease; factors contributing to the development of OA can include trauma (a single large trauma or many low-grade repetitive traumas), joint instability due to ligamentous injury, incongruent joint surfaces due to fractures or osteocondritis dissecans (OCD), and/or synovitis (inflammation of the joint). Inflammation in the joint can be particularly destructive, leading to damage to the joint even with normal weight-bearing forces. These insults to the joint lead to break down of the articular cartilage, which provides a smooth, cushioned surface for movement within the joint when healthy. Eventually the inflammation in the joint and destruction of the articular cartilage lead to remodelling of the bone, which can be diagnosed by radiographs. Because the detectable changes in the bone do not occur until after the cartilage is damaged, radiographs are not perfect diagnostic tools for detecting early OA, but are more valuable once the disease has progressed further.
Unfortunately, osteoarthritis is a progressive condition with no cure. Treatment focusses on prevention, controlling the symptoms, and slowing the progression of the disease. As this condition is multifactorial, there are many available treatment options, depending on the inciting cause and the severity of the disease. Controlling the inflammation is paramount to managing the horse’s comfort and slowing the progression of OA.
Oral non-steroidal anti-inflammatories such as phenylbutazone and previcox are one available option for decreasing inflammation throughout the horse’s body. These treatments are useful if there are a number of joints affected, the precise location of the arthritic pain has not been localized yet, the horse has a low degree of symptoms, or as an adjunctive therapy to other available treatments.
Oral joint supplements may also be useful; providing systemic doses of hyaluronic acid, glucosamine, MSM, and chondroitin, which all contribute to healthy joint fluid and cartilage components. Unfortunately, oral absorption of some of these molecules is variable between horses, and not every horse will respond well to only oral supplementation. Recent research has shown that treating horses with oral resveratrol (the anti-inflammatory molecule from red wine!) is successful in reducing the degree of lameness in horses with diagnosed OA, and supplements with this molecule are now becoming available.
Hyaluronic acid and polysulfated glycosaminoglycan are both components of healthy joint fluid and cartilage which are available in injectable forms – Legend and Adequan, respectively, are the most well-known brands of these medications. These medications provide some anti-inflammatory effect as well as improving the quality and health of the joint fluid and cartilage. They are most effective if used as an on-going monthly therapy, and can be used to treat multiple affected joints simultaneously.
The most direct therapy available for OA is intra-articular therapy targeted to the specific joints. A variety of products are available for intra-articular therapy, including the most commonly used combination of hyaluronic acid and corticosteroids. Other options for intra-articular therapy include products produced from the patient’s own blood or tissues: like IRAP, PRP, or stem cells. Targeted treatment of inflamed and painful joints is typically very effective and restores comfort while decreasing destructive inflammation in the affected joints. Depending on the severity of the OA in a particular joint, intra-articular therapy can last anywhere from 6 to 18 months.
Ultimately, the best approach for dealing with OA is as individual as the horse it affects. The most effective combination of the above listed therapies is best tailored to the specific case as determined by you and your veterinarian after a full lameness evaluation.
Contact us for a lameness exam if you have any concerns about your horse’s performance.
Laminitis, also referred to as founder, is a painful condition that can affect all hoofed animals, most commonly affecting horses and cattle. Laminitis is inflammation of the laminae, the structure within the horse’s feet that suspends the coffin bone from the hoof wall. This is a complex tissue composed of components of the hoof wall (the epidermis) and the dermal tissue closely associated with the coffin bone. These layers of tissue interlock with one another to form a tight hold between the hoof wall and the skeleton of the horse. When healthy, these interlocking tissues literally hold the horse up, suspending the skeleton within the hoof capsule, while still allowing the hoof wall to grow and slide past the stationary coffin bone. When the laminar tissues become inflamed, not only is it very painful for the horse to walk and stand on this inflamed tissue, but they lose their firm grip on one another. With the loss of firm attachment of the laminae, the coffin bone can begin to move within the hoof capsule. The movement of the coffin bone relative to the hoof wall is what is termed “founder” and comes in two varieties: rotation and sinking. Rotation is the more common type of founder, where the strong forces placed on the tendons at the back of the coffin bone pull the toe of the coffin bone down and away from the attachment to the hoof wall. Sinking describes downward movement of the skeleton within the hoof capsule without change in orientation relative to the hoof wall. Rotation and sinking can happen independent of one another, or simultaneously in the same hoof.
Laminitis can occur in any of the horse’s hooves but is most commonly seen in the forelimbs. Symptoms of laminitis include:
- Reluctance to walk, or even stand
- Reluctance to pick up one or both forelimbs, as weightbearing on the other limb is too painful
- Posturing in a “saw horse” stance, where the horse rocks their weight back onto their hindlimbs and extends their forelimbs in front of their body.
- Shifting weight between the left and right forelimbs, or hindlimbs
- Increased or “bounding” digital pulses (palpable at the lower back edges of the fetlocks)
- Heat in the affected hooves and coronary bands
- Painful response to hoof testers (a tool used by veterinarians and farriers to apply focal pressure to the hoof), particularly at the toe.
Causes of laminitis are variable, but are often related to one or more of the following causes:
- Over consumption of simple carbohydrates (grain or grass overload)
- Metabolic diseases like PPID (Cushing’s) or Insulin Resistance (see articles on both these diseases in our client education section for more detail)
- Septicemia (dramatic systemic infections)
- Severe diarrhea
- Retained placenta
- Increased weightbearing on one limb following injury to the contralateral limb, known as “supporting limb laminitis”
- Concussive trauma to the hoof, known as “road founder”
Treatment of acute laminitis is focussed on controlling and reducing the inflammation within the hooves. This is best done by a multi-faceted approach including anti-inflammatory medications like phenylbutazone and DMSO, cold therapy, supportive boots or pads, and restricted movement. Radiographs are useful to evaluate if any rotation or sinking of the coffin bone has occurred and determine the appropriate farriery adjustments required if so. Chronic laminitis treatment follows many of the same principles, with more of a focus on trimming and shoeing the affected hooves appropriately to support the damaged tissues and minimize the risk of recurrence. If you have any questions about your horse’s risk for developing laminitis, please contact our office to consult with a veterinarian.
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
Coming Soon!
